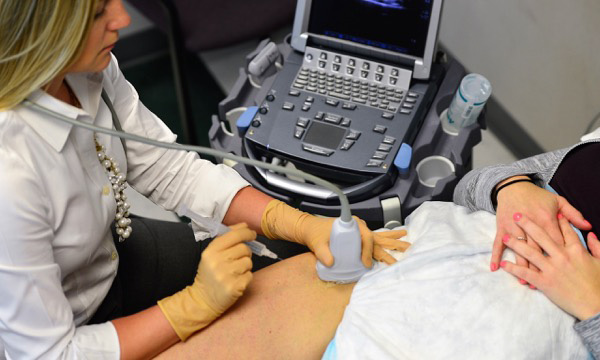
Hip Arthroscopy
(Learn More)
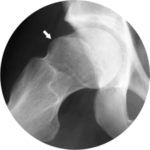
Femoroacetabular Impingement (FAI)
(Learn More)
Physical Therapy
(Learn More)
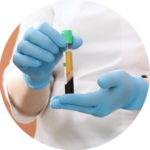
Orthobiologics
(Learn More)
J.W. Thomas Byrd, MD
Through the Nashville Hip Institute at TOA, Dr. Byrd brings more than 30 years of experience in treating complex hip disorders. His pioneering work in hip arthroscopy is the foundation upon which a multidisciplinary team has been assembled to treat hip problems with the latest non-surgical methods and most advanced arthroscopic techniques.
Our Mission
The mission of Nashville Hip Institute at TOA is to provide a highly integrated multidisciplinary team approach to treating hip problems, emphasizing the latest non-surgical and advanced arthroscopic techniques with a worldwide presence in education and research.
Comprehensive Hip Care & Sports Medicine
Every member of the care team at Nashville Hip Institute at TOA subspecializes in hip and orthopaedic disorders. Combining the talents of our Physical Therapists, Nurse Practitioners, Nurses, Athletic Trainers and OR team allows us to offer a comprehensive diagnostic and treatment plan to each individual patient, tailored to their unique experience with sports and orthopaedic injuries.
Hip Conditions
- Femoroacetabular Impingement (FAI)
- Pincer Impingement
- Cam Impingement
- Subspine Impingement
- Labrum & Articular Cartilage Injury
- Abductor Tendons (Gluteus Medius & Gluteus Minimus) Injury
- Snapping Hip Syndrome
- Ischiofemoral Impingement: The Other Snapping Hip
- Hamstring Injuries (Biceps Femoris, Semitendinosus & Semimembranosus)
- Piriformis Syndrome
- Trochanteric Bursitis / Greater Trochanteric Pain Syndrome (GTPS)
Hip Treatments
- Femoroacetabular Impingement (FAI) Treatment
- Femoroplasty
- Acetabular Rim Resection
- Subspine Impingement Treatment
- Labrum & Articular Cartilage: Repair, Chondroplasty & Microfracture
- Abductor Tendons (Gluteus Medius & Gluteus Minimus) Treatment
- Ilotibial Band Nonsurgical & Surgical Treatment
- Ischiofemoral Impingement Treatment
- Hamstring Injuries (Biceps Femoris, Semitendinosus & Semimembranosus) Treatment
- Piriformis Syndrome Treatment
- Trochanteric Bursitis / Greater Trochanteric Pain Syndrome (GTPS) Treatment
Telemedicine Services
Many of the greatest medical/surgical breakthroughs occur during times of war. Sadly, we are at war with a virus. At NHI at TOA we’re not saving lives (not yet), but we are trying to help people preserve their quality of life and careers. Within days, Telemedicine went from unheard of in our office, to part of our new daily norm.
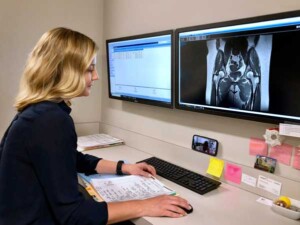
Follow-up Patient Care

Physical Therapy

New Patient Evaluation
Location
2004 Hayes Street
Suite 700
Nashville, TN 37203
Office Hours
Monday-Friday:
8:00 am – 5:00 pm